What are SCFA? 
SCFA stands for Short Chain Fatty Acids.
These are fatty acids that contain fewer than six carbon atoms in their chemical structure.
https://www.nature.com/articles/s41577-024-01014-8
The most prominent SCFAs found in the human gut are
- Acetate (C2)
- Propionate (C3)
- Butyrate (C4)
Butyrate specifically refers to butyric acid, a type of SCFA with four carbon atoms.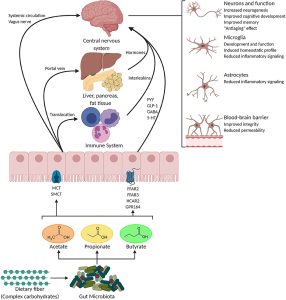
Butyrate plays several crucial roles in the body, especially in the gastrointestinal tract.
- Evidence is accumulating that short chain fatty acids (SCFA) play an important role in the maintenance of gut and metabolic health.
- The SCFA acetate, propionate, and butyrate are produced from the microbial fermentation of indigestible carbohydrates and appear to be key mediators of the beneficial effects elicited by the gut microbiome.
- Microbial SCFA production is essential for gut integrity by regulating the luminal pH, mucus production, providing fuel for epithelial cells, and effects on mucosal immune function.
- SCFA also directly modulate host metabolic health through a range of tissue-specific mechanisms related to appetite regulation, energy expenditure, glucose homeostasis, and immunomodulation.
- Increased microbial SCFA production can be considered a health benefit, but data are mainly based on animal studies, whereas well-controlled human studies are limited.
- An expert group by ILSI Europe’s Prebiotics Task Force discussed the current scientific knowledge on SCFA to consider the relationship between SCFA and gut and metabolic health with a particular focus on human evidence.
- Overall, the available mechanistic data and limited human data on the metabolic consequences of elevated gut-derived SCFA production strongly suggest that increasing SCFA production could be a valuable strategy in preventing gastro-intestinal dysfunction, obesity, and type 2 diabetes mellitus.
- Nevertheless, there is an urgent need for well-controlled longer-term human SCFA intervention studies, including measurement of SCFA fluxes and kinetics, the heterogeneity in response based on metabolic phenotype, the type of dietary fiber and fermentation site in fiber intervention studies, and the control for factors that could shape the microbiome like diet, physical activity, and use of medication.
https://pubmed.ncbi.nlm.nih.gov/32865024/
It serves as a primary energy source for the cells lining the colon (colonocytes) and plays a role in maintaining gut barrier integrity, reducing inflammation, and regulating immune function.
The mechanism of action of butyrate involves its interaction with various receptors and pathways within the gastrointestinal tract.
One important mechanism is its role as a histone deacetylase (HDAC) inhibitor, which can regulate gene expression and influence cellular processes such as proliferation and differentiation.
Butyrate also acts on specific receptors such as GPR43 and GPR109A, which are involved in signaling pathways related to inflammation and metabolism.
SCFA: mechanisms and functional importance in the gut
- In recent years, the importance of the gut microbiota in human health has been revealed, highlighting its role as a key component of human physiology.
- Modern sequencing approaches have allowed for the characterization of the microbiome in healthy individuals and in disease, demonstrating a disturbance of the microbiota, or dysbiosis, associated with pathological conditions.
- The microbiota establishes a symbiotic crosstalk with their host: commensal microbes benefit from the nutrient-rich environment provided by the gut, and the microbiota produces hundreds of proteins and metabolites that modulate key functions of the host, including nutrient processing, maintenance of energy homeostasis, and immune system development.
- Many bacteria-derived metabolites originate from dietary sources, with an important role attributed to the metabolites derived from the bacterial fermentation of dietary fibers, namely short-chain fatty acids (SCFA), linking host nutrition to intestinal homeostasis maintenance.
- SCFA are important fuels for intestinal epithelial cells (IEC) and regulate IEC functions through different mechanisms, modulating their proliferation, differentiation, and functions of subpopulations such as enteroendocrine cells, impacting gut motility, and strengthening gut barrier functions as well as host metabolism.
- Recent findings show that SCFA, particularly butyrate, also have important intestinal and immuno-modulatory functions.
- The review discusses the mechanisms and the impact of SCFA on gut functions and host immunity, consequently affecting human health.
https://pubmed.ncbi.nlm.nih.gov/32238208/
The purpose of butyrate in the body includes:
- Providing energy: Butyrate is a significant energy source for the cells lining the colon, contributing to their function and maintenance.
- Maintaining gut barrier integrity: Butyrate helps strengthen the intestinal barrier, which is crucial for preventing the entry of harmful substances into the bloodstream.
- Modulating inflammation: Butyrate exhibits anti-inflammatory properties, helping to reduce inflammation in the gut and throughout the body.
- Regulating immune function: Butyrate influences immune cell activity and helps maintain a balance between immune tolerance and response.
Ways to improve butyrate levels in the body include:
- Diet: Consuming foods rich in dietary fiber, particularly those that contain resistant starches and non-digestible carbohydrates, can promote the production of butyrate by gut bacteria.
- Probiotics and prebiotics: Certain probiotic bacteria and prebiotic fibers can stimulate the production of butyrate by promoting the growth of butyrate-producing bacteria in the gut.
- Butyrate supplementation: In some cases, supplementation with butyrate or butyrate-producing compounds may be beneficial, although more research is needed to determine its effectiveness and safety.
When butyrate levels are too low:
-
- it can lead to various gastrointestinal issues and may contribute to conditions such as inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), and colorectal cancer.
- Symptoms of low butyrate levels may include increased intestinal permeability, inflammation, and alterations in gut microbiota composition.
Low levels of butyrate and other SCFAs can lead to various symptoms and health issues due to their crucial roles in maintaining gut health and overall wellbeing.

