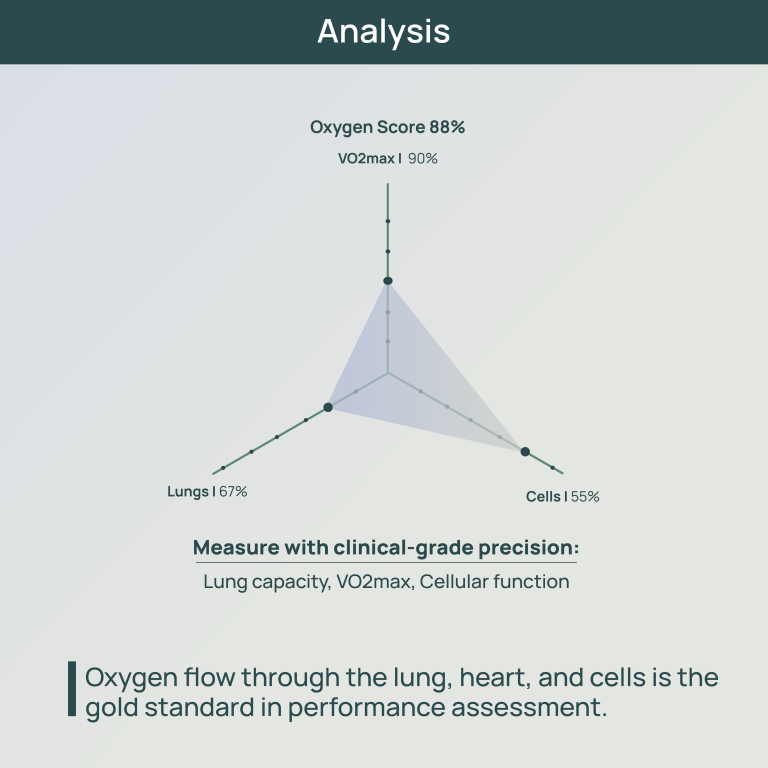
Test and not Guess how you should fuel, train and perform each day!
Which lifestyle habits, hacks and stacked hacks are necessary for YOU?
- Use science – not math – to identify zones
- Metabolic analysis gives you the most accurate method of identifying training zones
- Accurate intensity zones are vital to developing effective training plans (FITT)
- We use multiple metrics to accurately identify your zones
- Ensure you help your customers employ our zones into their training plans
- e.g. Garmin and Polar allow users to set their own zones manually
- Zones change significantly when effective exercise programming is prescribed (and completed) and therefore you must retest regularly to measure your customers changes in limitation(s) and zoning so you can adjust your customers training focus and their intensities appropriately
STRUCTURAL VS.FUNCTIONAL TRAINING
- Testing identifies which structures are leading to performance limitations
- Train them at the exercise intensity (zones) and frequency, type and time required to AFFECT THEIR LIMITING STRUCTURES and thereby minimize or eliminate their limitation
- IF there is no limiting structure – TRAIN FUNCTION
Are you getting the correct assessment to have a personalized fueling, training and performance program based on science??

What is a metabolically healthy individual in functional medicine?
A metabolically healthy individual typically has balanced blood sugar levels, efficient energy production, proper hormone regulation, and effective detoxification mechanisms. Functional medicine practitioners often assess various markers of metabolic health, such as insulin sensitivity, inflammation levels, lipid profiles, and gut function.
Key factors considered in evaluating metabolic health in functional medicine may include:
- Blood Sugar Regulation: Maintaining stable blood sugar levels is crucial for metabolic health. Individuals with good metabolic health typically have insulin sensitivity, meaning their cells respond appropriately to insulin, which helps regulate blood sugar.
- Energy Production: Efficient energy production is a sign of a healthy metabolism. This involves the proper functioning of mitochondria, the cellular structures responsible for generating energy.
- Hormone Balance: Hormones play a crucial role in metabolic regulation. Imbalances in hormones such as insulin, cortisol, thyroid hormones, and sex hormones can impact metabolic health.
- Inflammation Levels: Chronic inflammation is often associated with metabolic dysfunction. Functional medicine practitioners may assess inflammatory markers to understand the level of inflammation in the body.
- Lipid Profile: A balanced lipid profile, including levels of cholesterol and triglycerides, is important for cardiovascular health and is often considered in assessing metabolic health.
- Gut Health: The gut is closely linked to overall health, including metabolism. A well-functioning digestive system and a balanced gut microbiome contribute to metabolic health.
Functional medicine aims to optimize these factors through personalized and integrative approaches, which may include dietary changes, lifestyle modifications, targeted supplementation, stress management, and other interventions tailored to the individual’s specific needs.
It’s important to note that the concept of metabolic health in functional medicine is a comprehensive and individualized approach that goes beyond conventional medicine’s focus on disease management. Instead, it emphasizes proactive measures to promote overall well-being and prevent the development of chronic health issues.
What is a fat adapted endurance athlete?
A fat-adapted endurance athlete is an individual whose metabolism has adapted to efficiently utilize fat as a primary source of energy during prolonged physical activities, particularly in endurance sports. This adaptation allows athletes to rely on stored fat for fuel, which can be beneficial for maintaining energy levels over extended periods without relying heavily on carbohydrates.
In a typical scenario, the body primarily uses carbohydrates (glycogen) as a quick and accessible source of energy during high-intensity exercise. However, glycogen stores are limited, and for longer-duration activities, such as marathon running, triathlons, or long-distance cycling, relying solely on carbohydrates may lead to “hitting the wall” or fatigue due to glycogen depletion.
Fat adaptation involves training the body to become more efficient at burning fat for energy, sparing glycogen for higher-intensity efforts. This adaptation is often achieved through dietary and training strategies. Some key elements of becoming a fat-adapted endurance athlete include:
- Low-Carbohydrate, High-Fat (LCHF) Diet: Adopting a diet that is lower in carbohydrates and higher in healthy fats can encourage the body to rely more on fat for fuel. This type of diet might include sources of healthy fats such as avocados, nuts, seeds, and oils.
- Endurance Training: Incorporating low to moderate-intensity, long-duration training sessions into the workout routine can stimulate the body to become more efficient at burning fat. These sessions are often referred to as “fat-burning” or “aerobic base” workouts.
- Periodic Fasting: Intermittent fasting or occasional longer fasting periods can also promote fat adaptation by encouraging the body to tap into its fat stores for energy.
- Strategic Carbohydrate Intake: While the overall carbohydrate intake may be lower, strategically incorporating carbohydrates during and after high-intensity training sessions or competitions can help support glycogen stores during these specific times.
It’s important to note that the process of becoming a fat-adapted athlete is individual, and what works for one person may not work the same way for another. Additionally, fat adaptation doesn’t mean complete exclusion of carbohydrates but rather optimizing the body’s ability to use both fats and carbohydrates efficiently.
Some athletes and coaches believe that being fat-adapted may have advantages in terms of prolonged endurance performance and avoiding the “bonk” or hitting a wall during extended activities. However, research in this area is ongoing, and individual responses to different dietary and training approaches can vary. Athletes interested in becoming fat-adapted often work closely with sports nutritionists or coaches to tailor their approach to their specific needs and goals.
Nutritional ketosis is a metabolic state in which the body shifts from primarily using glucose as its main source of energy to relying on ketones, which are molecules produced from the breakdown of fats. This state is achieved through a low-carbohydrate, high-fat diet, commonly known as a ketogenic diet.
When carbohydrate intake is significantly reduced, the body’s glycogen stores become depleted. In the absence of glucose, the liver increases the production of ketones from fatty acids. These ketones, particularly beta-hydroxybutyrate, acetoacetate, and acetone, become an alternative fuel source for various tissues, including the brain.
Key features of nutritional ketosis include:
- Low Carbohydrate Intake: To induce nutritional ketosis, carbohydrate intake is typically restricted to a very low level, usually around 20-50 grams of net carbs per day. This restriction leads to reduced blood glucose levels and insulin secretion.
- Moderate Protein Intake: Protein intake is moderate and is adjusted based on individual needs. Consuming excessive protein can potentially interfere with ketone production through a process called gluconeogenesis, where the body converts protein into glucose.
- High Fat Intake: The majority of daily caloric intake comes from healthy fats, such as avocados, nuts, seeds, oils, and fatty fish. This high fat intake provides the body with the necessary building blocks for ketone production.
- Ketone Production: As carbohydrate intake decreases, the liver starts producing ketones, which can be measured in the blood, urine, or breath. Elevated ketone levels are a sign that the body is in a state of nutritional ketosis.
Nutritional ketosis is different from diabetic ketoacidosis, which is a dangerous condition that can occur in people with uncontrolled diabetes. In nutritional ketosis, ketone levels are moderate and well-regulated, providing a stable and efficient energy source.
People may pursue nutritional ketosis for various reasons, including weight loss, improved mental clarity, enhanced athletic performance, and potential therapeutic benefits for certain health conditions. It’s important to note that nutritional ketosis may not be suitable for everyone, and individuals considering this dietary approach should consult with healthcare professionals or nutrition experts to ensure it aligns with their health goals and is implemented safely.
 Dr. Dan Plews:
Dr. Dan Plews:
- Dr. Dan Plews is known for his work in sports science and coaching, particularly in the area of endurance sports.
- Dr. Plews, along with his colleague Dr. Paul Laursen, has developed the concept of “The Low Carb, High Fat (LCHF) approach” for endurance athletes, which involves promoting fat adaptation through a ketogenic or low-carbohydrate diet.
- Their research suggests that becoming fat-adapted, where the body becomes more efficient at utilizing fat for fuel, may have potential benefits for endurance athletes, especially in prolonged activities.
- Dr. Stacy Sims:
- Dr. Stacy Sims is a researcher and exercise physiologist known for her work on sex differences in training, nutrition, and environmental conditions for athletes.
- While Dr. Sims acknowledges the potential benefits of low-carbohydrate and ketogenic diets for certain individuals, she emphasizes the importance of considering the individual athlete’s needs, including hormonal differences between men and women.
- Dr. Sims has highlighted the importance of menstrual cycle considerations in female athletes and has discussed the concept of “women are not small men” in terms of training and nutrition.
It’s essential to recognize that the effectiveness of nutritional ketosis or low-carbohydrate approaches can vary among individuals. Athletes have different responses to dietary strategies, and factors such as training intensity, duration, and personal preferences play a role.
For the most current and accurate information on the recommendations of Dr. Dan Plews and Dr. Stacy Sims regarding nutritional ketosis for endurance athletes, I recommend checking their official websites, recent publications, or consulting with them directly if possible. Additionally, reviewing the latest research in the field of sports nutrition can provide valuable insights into evolving perspectives on this topic
Systems and Fuel Sources
Aerobic Sources
- Free fatty acids (beta oxidation – Krebs cycle)
- Carbohydrates (CHO)
- Amino acids (protein) if required
- By product of glycolysis (pyruvate to oxidated lactate) then though
Krebs cycle and electron transport chain
Anaerobic Sources
- Stored ATP
- Phosphocreatine (CrP)
- Glucose – CHO (phosphorylation)
- Many different names for the same systems
- Anaerobic alactic or phosphagen or ATP PC for CrP
Zoning is based upon changes in FUEL SOURCES. You must be able to identify at what intensity YOU change from one PRIMARY energy system to another which can be identified by recognizing changes in VO2, VCO2 and respiration – all available through metabolic analysis.
How does NADH and NAD+ play a role in exercise metabolism to create ATP for energy?
NADH (nicotinamide adenine dinucleotide) and NAD+ (the oxidized form of NADH) play crucial roles in exercise metabolism, particularly in the process of cellular respiration, which is the primary way cells generate ATP (adenosine triphosphate), the energy currency of the cell.
Here’s a simplified explanation of how NADH and NAD+ function in exercise metabolism for ATP production:
- Glycolysis:
- During the early stages of exercise, when oxygen availability is limited (as in anaerobic exercise), the breakdown of glucose begins with glycolysis in the cytoplasm.
- NAD+ is required as a coenzyme in the glycolytic pathway to facilitate the conversion of glucose into pyruvate.
- In the process, NAD+ is reduced to NADH when it accepts electrons from glycolytic intermediates.
- Pyruvate Decarboxylation:
- If oxygen is available (as in aerobic exercise), pyruvate produced during glycolysis enters the mitochondria.
- In the mitochondrial matrix, pyruvate is further oxidized through a process called pyruvate decarboxylation.
- NAD+ is again involved as a coenzyme in this process, accepting electrons from the breakdown of pyruvate and forming NADH.
- Citric Acid Cycle (Krebs Cycle):
- Acetyl-CoA, the product of pyruvate decarboxylation, enters the citric acid cycle.
- In the citric acid cycle, NAD+ is once again reduced to NADH as electrons are transferred from various intermediates to NAD+.
- Electron Transport Chain (ETC):
- NADH generated in glycolysis, pyruvate decarboxylation, and the citric acid cycle transfers its electrons to the electron transport chain, located in the inner mitochondrial membrane.
- The electrons move through the electron transport chain, releasing energy that is used to pump protons across the inner mitochondrial membrane, creating a proton gradient.
- ATP Synthesis:
- The proton gradient created in the electron transport chain is used to drive ATP synthesis through a process called oxidative phosphorylation.
- NADH donates its electrons to the electron transport chain, ultimately leading to the regeneration of NAD+.
- The flow of protons back into the mitochondrial matrix through ATP synthase results in the synthesis of ATP from ADP and inorganic phosphate.
In summary, NADH is produced during the initial stages of glucose breakdown, and its electrons are used to generate a proton gradient that drives ATP synthesis during oxidative phosphorylation. NAD+ is crucial for maintaining the flow of electrons in these metabolic pathways. This process is central to the efficient production of ATP during exercise, especially in aerobic conditions.
Difference between Lactate and Lactic Acid
- Lactate is a biproduct of glycolysis (anaerobic) and is a FUEL in the presence of oxygen so therefore DEPENDENT upon your aerobic system
- Lactic acid breaks down into lactate and a hydrogen ion…is it the hydrogen ion that causes the acidosis that drives increased respiration
- Hydrogen ions are used in the electron transport chain to create
ATP and H20 and CO2 - Lactic acid usually blamed for muscle soreness due to acidosis, but it is the accumulation of H+ that has been identified as one of the main causes for the pH change (acidosis) and muscle fatigue

- The the aerobic metabolism and respiratory systems are the MOST important systems for being able to process H+ ions and lactate and maintain the pH and therefore continue exercise at high intensity
“Anaerobic breakdown of glycogen leads to an intracellular accumulation of inorganic acids, of which lactic acid is quantitatively the most important. Since lactic acid is a strong acid, it dissociates into lactate and H*. Lactate ions would have little effect on muscle contraction; however, the increase in H* (i.e., reduced pH or acidosis) is the classic cause of skeletal muscle fatigue. However, the role of reduced pH as an important cause of fatigue is now being challenged, and several recent studies show that reduced pH may have little effect on contraction in mammalian muscle at physiological temperatures.” Or does the body maintain pH well through the use of H+ through the electron transport chain or extraction of H+ through your respiratory system through CO2 expulsion
How can you improve your mitochondria function & reduce oxidative stress?
Improving mitochondrial biogenesis and reducing oxidative stress are two interconnected goals that contribute to overall cellular health and function. Here are some lifestyle and dietary strategies that may help achieve these objectives:
1. Regular Exercise:
- Aerobic Exercise: Regular aerobic exercise has been shown to enhance mitochondrial biogenesis. Activities like running, cycling, and swimming stimulate the production of new mitochondria.
- Resistance Training: Strength training also has positive effects on mitochondrial function.
2. High-Intensity Interval Training (HIIT):
- HIIT has been shown to be particularly effective in promoting mitochondrial biogenesis and improving overall metabolic health.
3. Balanced Nutrition:
- Antioxidant-Rich Diet: Include a variety of fruits and vegetables rich in antioxidants, such as vitamins C and E, to combat oxidative stress.
- Omega-3 Fatty Acids: Consuming foods high in omega-3 fatty acids, like fatty fish and flaxseeds, may help reduce inflammation and oxidative stress.
- Polyphenol-Rich Foods: Foods rich in polyphenols, such as green tea, berries, and dark chocolate, have antioxidant properties.
4. Intermittent Fasting:
- Some studies suggest that intermittent fasting may stimulate mitochondrial biogenesis and improve mitochondrial function.
5. Adequate Sleep:
- Lack of sleep can contribute to oxidative stress. Ensure you get sufficient, quality sleep each night.
6. Stress Management:
- Chronic stress can contribute to oxidative stress. Practice stress-reducing techniques such as meditation, deep breathing, or yoga.
7. Supplements:
- Coenzyme Q10 (CoQ10): CoQ10 is a compound that plays a crucial role in mitochondrial function and may have antioxidant properties.
- N-Acetyl Cysteine (NAC): NAC is a precursor to glutathione, a potent antioxidant that helps reduce oxidative stress.
- Resveratrol: Found in red grapes and berries, resveratrol has been studied for its potential to enhance mitochondrial function and reduce oxidative stress.
8. Avoid Excessive Caloric Intake:
- Caloric excess can lead to oxidative stress. Maintaining a healthy weight through a balanced diet and regular exercise is essential.
9. Cold Exposure (Cryotherapy):
- Cold exposure has been suggested to stimulate mitochondrial biogenesis. This can include cold showers or exposure to cold environments.
10. Regular Health Check-ups:
- Monitor and manage conditions such as diabetes and hypertension, as these can contribute to oxidative stress.
It’s important to note that individual responses may vary, and consulting with a healthcare professional or a registered dietitian is recommended before making significant changes to your exercise routine, diet, or supplementation. They can provide personalized guidance based on your specific health status and goals.